 (2012) showed that mild to moderate increases in hematocrit and blood viscosity did not result in a rise in vascular resistance or blood pressure, but actually caused the opposite effect. One of the most important molecules that promotes an augmentation in vascular diameter (i.e., vasodilation) is nitric oxide (NO). This is because vessels are not rigid tubes they can change their diameters in response to various physiological stimuli. However, several works conducted in the past 10–15 years have shown that, in a physiological context, the parameters of this equation cannot be considered to be truly independent of each other. The dimensions of the vascular system (most notably the radius, which is raised to the fourth power) play a more important role in determining vascular resistance than blood viscosity does. When applying Poiseuille’s Law to the cardiovascular system, one must consider the radius and the length of the vessels, and the viscosity of the blood. Moreover, regular physical exercise has been shown to decrease blood viscosity in sickle cell mice, which could be beneficial for adequate blood flow and tissue perfusion. While acute, intense exercise may increase blood viscosity in healthy individuals, recent works conducted in sickle cell patients have shown that light cycling exercise did not cause dramatic changes in blood rheology. This paradox seems to be due to the fact that in SCD RBC with the highest deformability are also the most adherent, which would trigger vaso-occlusion. However, while the deformability of RBC decreases during acute vaso-occlusive events in SCD, patients with the highest RBC deformability at steady-state have a higher risk of developing frequent painful vaso-occlusive crises. We previously showed that sickle cell patients with high blood viscosity usually have more frequent vaso-occlusive crises than those with low blood viscosity. In this context, any increase in blood viscosity can promote vaso-occlusive like events. However, in sickle cell disease (SCD) vascular function is impaired. This is the case in healthy individuals when vascular function is intact and able to adapt to blood rheological strains. Indeed, any increase in blood viscosity should promote vasodilation. However, blood viscosity, through its effects on wall shear stress, is a key modulator of nitric oxide (NO) production by the endothelial NO-synthase. Poiseuille’s Law predicts that any increase in blood viscosity should cause a rise in vascular resistance.  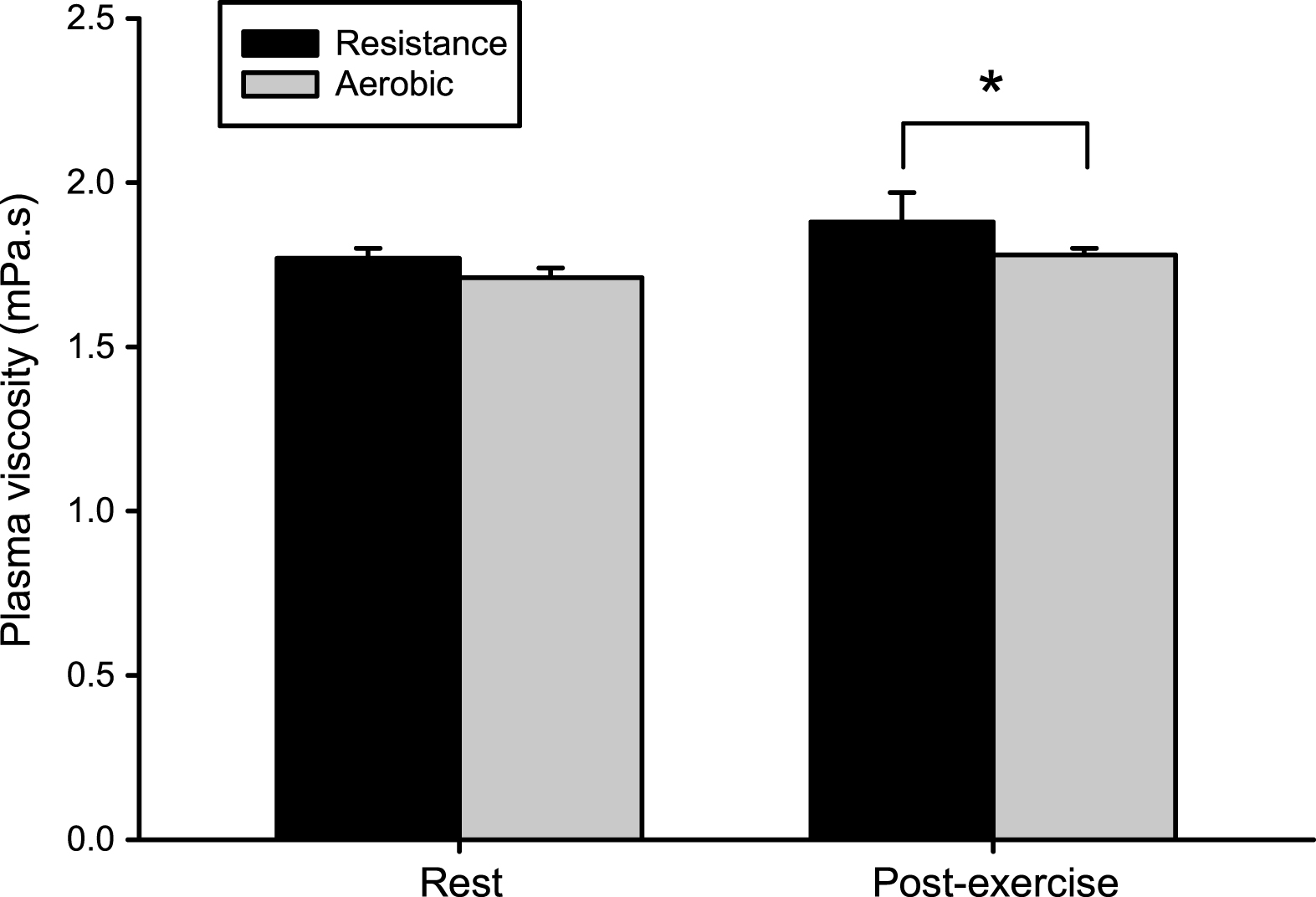
Indeed, any changes in one or several of these parameters may affect blood viscosity differently. Blood flow in the microcirculation is highly dependent on the ability of RBC to deform, but RBC deformability also affects blood flow in the macrocirculation since a loss of deformability causes a rise in blood viscosity. RBC aggregation occurs at low shear rates, and increases blood viscosity and depends on both cellular (RBC aggregability) and plasma factors. The shear thinning property of blood is mainly attributed to red blood cell (RBC) rheological properties. Both hematocrit and plasma viscosity influence blood viscosity. 11Centre de Médecine du Sommeil et des Maladies Respiratoires, Hospices Civils de Lyon, Hôpital de la Croix Rousse, Lyon, Franceīlood viscosity is an important determinant of local flow characteristics, which exhibits shear thinning behavior: it decreases exponentially with increasing shear rates.10Laboratoire de Biochimie et de Biologie Moleìculaire, UF de Biochimie des Pathologies Eìrythrocytaires, Centre de Biologie et de Pathologie Est, Hospices Civils de Lyon, Lyon, France.9Laboratoire ACTES EA 3596, The Université des Antilles, Pointe-a-Pitre, France.8d’Hématologie et d’Oncologie Pédiatrique, Hospices Civils de Lyon, Lyon, France.7Laboratoire Carmen INSERM 1060, INSA Lyon, Université Claude Bernard Lyon 1, Université de Lyon, Villeurbanne, France.6Unité Transversale de la Drépanocytose, Hôpital de Pointe-a-Pitre, Hôpital Ricou, Pointe-a-Pitre, France. 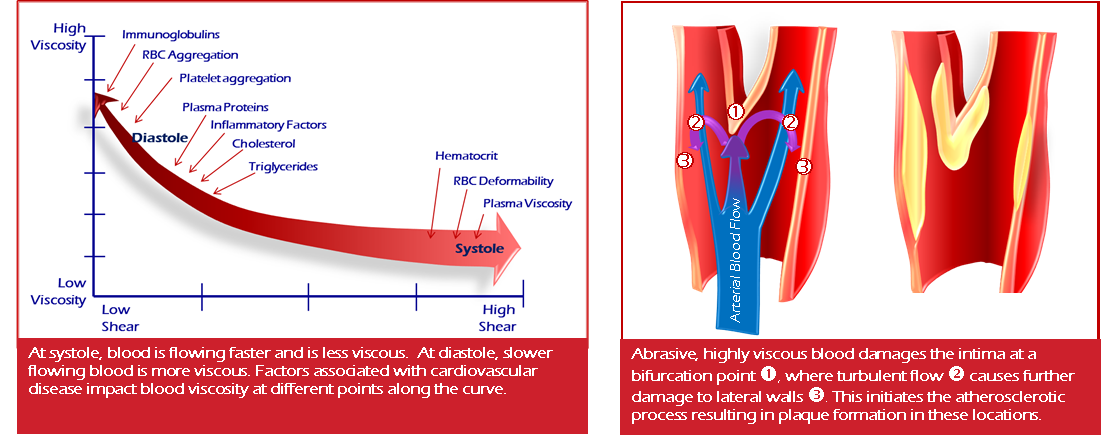
5Département de Médecine, Hôpital Edouard Herriot, Hospices Civils de Lyon, Lyon, France.4Biologie Intégrée du Globule Rouge, The Université des Antilles, UMR_S1134, BIGR, F- 97157, Pointe-a-Pitre, France.3Biologie Intégrée du Globule Rouge, Université de Paris, UMR_S1134, BIGR, INSERM, F-75015, Paris, France.2Laboratory of Excellence GR-Ex, Paris, France.1Laboratory LIBM EA7424, Team “Vascular Biology and Red Blood Cell”, University of Lyon 1, Lyon, France.Elie Nader 1,2† Sarah Skinner 1,2† Marc Romana 2,3,4 Romain Fort 1,2,5 Nathalie Lemonne 6 Nicolas Guillot 7 Alexandra Gauthier 1,2,8 Sophie Antoine-Jonville 9 Céline Renoux 1,2,10 Marie-Dominique Hardy-Dessources 2,3,4 Emeric Stauffer 1,2,11 Philippe Joly 1,2,10 Yves Bertrand 8 Philippe Connes 1,2* 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
